Intermittent fasting (IF) has transcended the realm of dietary trends to become a significant area of scientific inquiry, lauded for its potential benefits in weight management, cellular repair, and metabolic health. However, beyond the scale, a more intricate conversation is unfolding—one that centers on the profound connection between fasting and the body’s complex endocrine system. This article explores the nuanced relationship between intermittent fasting and hormonal balance, delving into the evidence-based impacts on key hormones and offering practical guidance for those looking to harmonize their health.
Understanding Intermittent Fasting

At its core, intermittent fasting is not about what you eat, but when you eat. It involves cycling between periods of voluntary fasting and non-fasting over a given timeframe. The most common protocols include:
•Time-Restricted Feeding (TRF): This popular approach involves consuming all daily calories within a specific window, typically 6-10 hours, and fasting for the remaining 14-18 hours. The 16/8 method is a classic example.
•Alternate-Day Fasting (ADF): This protocol involves alternating between days of normal eating and days of complete or significant calorie restriction (often around 500 calories).
•The 5:2 Diet: This method involves eating normally for five days of the week and restricting calorie intake to approximately 500-600 calories on two non-consecutive days.
These structured eating patterns trigger a cascade of metabolic and hormonal adjustments as the body shifts from using glucose as its primary fuel source to tapping into stored fat.
The Endocrine System: A Symphony of Signals
Our hormonal system is an intricate network of glands and chemical messengers that regulate nearly every bodily function, from metabolism and growth to mood and reproduction. Hormones like insulin, cortisol, and growth hormone operate in a delicate, often circadian-driven rhythm. When this balance is disrupted, it can lead to a host of health issues, including metabolic syndrome, thyroid dysfunction, and reproductive challenges. The central question, therefore, is whether intermittent fasting acts as a conductor, restoring harmony to this hormonal symphony, or as a disruptive force.
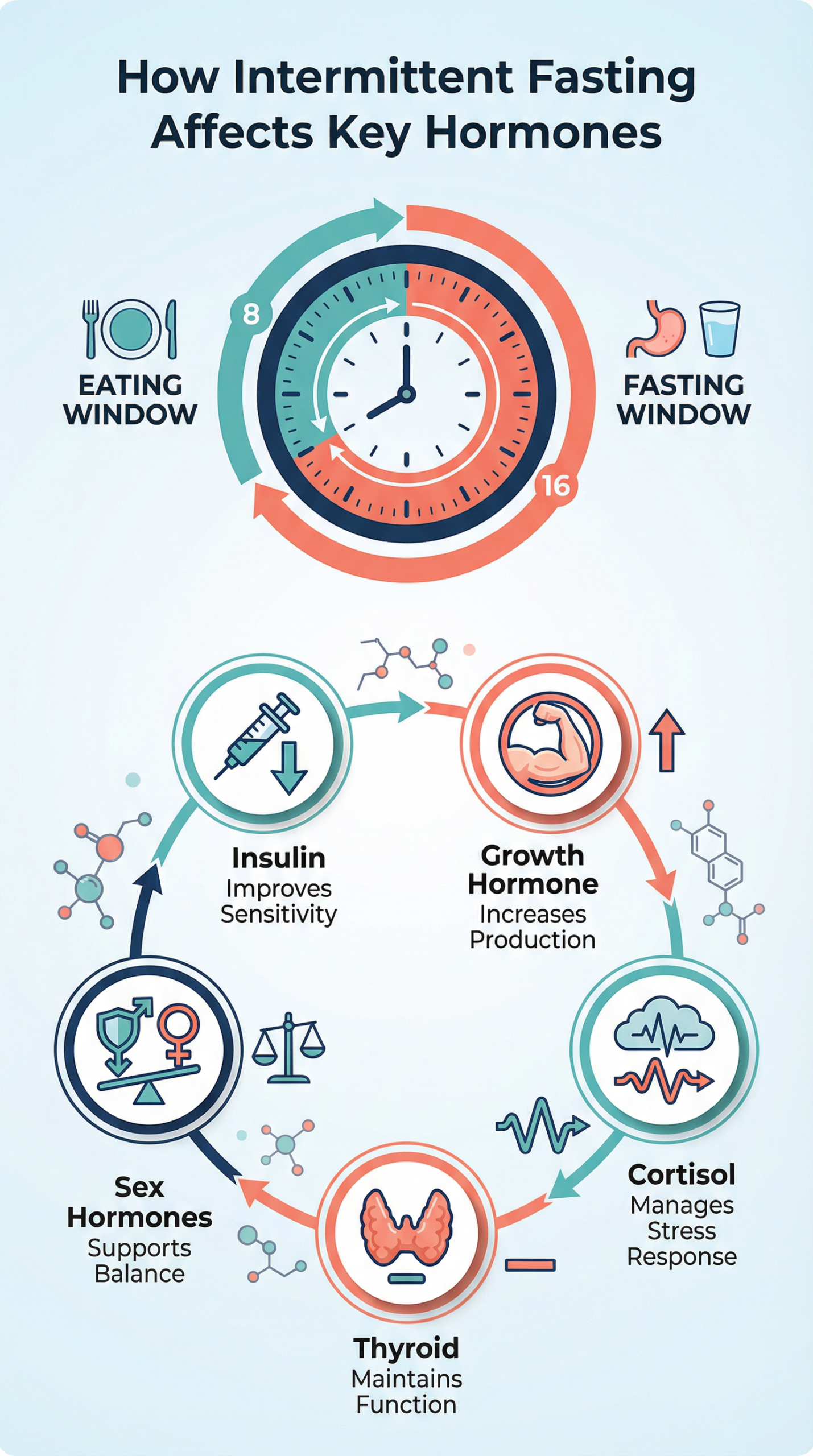
Intermittent Fasting’s Impact on Key Hormones
Scientific research reveals that fasting is a powerful modulator of the endocrine system. The effects are multifaceted, with significant implications for several key hormones.
Insulin: The Metabolic Master Switch
Perhaps the most well-documented effect of intermittent fasting is its impact on insulin, the hormone responsible for regulating blood sugar. When we eat, insulin levels rise to shuttle glucose into cells for energy. Persistently high insulin levels, often a result of frequent eating and high-carbohydrate diets, can lead to insulin resistance—a precursor to type 2 diabetes.
Intermittent fasting provides a crucial metabolic break. During fasting periods, insulin levels drop significantly. Studies have shown that this decline can be dramatic; for instance, some research indicates that 72 hours of fasting can cut plasma insulin levels in half . Other protocols, like the 5:2 diet and alternate-day fasting, have demonstrated a significant reduction in both baseline insulin levels and insulin resistance, often independent of total calorie reduction . By improving insulin sensitivity, IF allows the body to manage blood sugar more effectively, reducing the risk of metabolic disease and facilitating fat loss.
Human Growth Hormone (HGH): The Repair and Rejuvenation Hormone
Human Growth Hormone plays a vital role in growth, cell repair, and metabolism. It helps to build and maintain lean muscle mass while encouraging the body to use fat for fuel. Interestingly, fasting is one of the most potent natural stimuli for HGH secretion. Research has found that fasting periods can lead to substantial, albeit temporary, increases in HGH levels . This surge in HGH during a fast is a key adaptive mechanism, helping to preserve muscle tissue and promote cellular repair processes like autophagy, where the body clears out damaged cells and proteins.
Cortisol: The Stress and Energy Mobilizer
The relationship between intermittent fasting and cortisol, the body’s primary stress hormone, is complex. Cortisol follows a natural circadian rhythm, peaking in the morning to promote wakefulness and gradually declining throughout the day. Fasting is a form of hormetic stress—a mild, beneficial stressor that can strengthen the body’s resilience.
During a fast, cortisol levels naturally rise to help mobilize stored glucose and fat for energy . This is a normal and necessary adaptive response. However, the concern lies with the potential for chronic cortisol elevation, especially with prolonged or overly aggressive fasting protocols. Persistently high cortisol can lead to muscle breakdown, increased belly fat, and hormonal dysregulation. This is particularly crucial for women, whose hormonal systems can be more sensitive to stress signals. Therefore, managing overall stress and avoiding excessive fasting is key to keeping cortisol’s role beneficial rather than detrimental.
Thyroid Hormones: The Metabolic Thermostat
Thyroid hormones (T3 and T4) are critical for regulating the body’s metabolic rate. Some concerns have been raised about whether fasting could suppress thyroid function as a mechanism to conserve energy. Prolonged fasting has been shown to blunt the response of Thyroid-Stimulating Hormone (TSH) . However, most standard intermittent fasting protocols, particularly time-restricted feeding, do not appear to negatively impact thyroid function in healthy individuals. Those with pre-existing thyroid conditions should, however, approach fasting with caution and under medical supervision.
Sex Hormones: A Gendered Response
The impact of intermittent fasting on sex hormones like estrogen and testosterone is an area of active research, and the response can differ between men and women. Some studies suggest that IF may decrease androgen markers in women while increasing sex hormone-binding globulin (SHBG), which could be beneficial in conditions like Polycystic Ovary Syndrome (PCOS) . For men, some research points to potential increases in luteinizing hormone and testosterone, though more studies are needed.
Women, in particular, need to be mindful of how fasting fits within their menstrual cycle, as the female reproductive system is highly sensitive to energy availability. Fasting during certain phases of the cycle may be more beneficial than others.
Practical Tips for Supporting Hormonal Balance with IF

For those looking to explore intermittent fasting, the goal is to reap the benefits without disrupting hormonal harmony. The following tips can help guide a balanced approach:
1.Start Slowly: If you are new to fasting, begin with a shorter fasting window, such as 12-14 hours, and gradually extend it as your body adapts. Avoid jumping into prolonged or aggressive fasts.
2.Prioritize Nutrient Density: The quality of your food is paramount. During your eating window, focus on a whole-foods diet rich in protein, healthy fats, fiber, and micronutrients to support hormonal production and overall health.
3.Stay Hydrated: Drink plenty of water, herbal tea, or black coffee during your fasting period to stay hydrated and manage hunger.
4.Listen to Your Body: Pay close attention to your energy levels, mood, sleep quality, and (for women) menstrual cycle. If you experience persistent negative symptoms like fatigue, irritability, or sleep disturbances, it may be a sign to shorten your fast or take a break.
5.Manage Overall Stress: Since fasting is a stressor, it is crucial to manage other sources of stress in your life through practices like mindfulness, yoga, adequate sleep, and gentle exercise.
Conclusion: A Personalized Path to Hormonal Health
Intermittent fasting is a powerful dietary strategy with the potential to significantly improve metabolic health by recalibrating key hormonal pathways. Its ability to enhance insulin sensitivity, boost growth hormone, and align our bodies with their natural circadian rhythms offers a compelling therapeutic tool. However, it is not a panacea. The body’s endocrine system is a finely tuned instrument, and the impact of fasting can vary based on an individual’s age, sex, genetics, and underlying health status.
A successful approach to intermittent fasting is one that is personalized, flexible, and mindful of the body’s intricate hormonal feedback loops. By starting slowly, focusing on nutrient quality, and listening to your body’s signals, you can navigate the rhythm of fasting to unlock profound benefits for hormonal balance and long-term well-being.