Menopause brings enough challenges on its own—hot flashes, sleep disruption, mood changes. But when chronic stress enters the picture, it creates a particularly difficult combination for weight management.
The connection isn’t just coincidental. Stress triggers specific hormonal responses that directly affect where your body stores fat, what foods you crave, and how your metabolism functions. During menopause, when hormonal changes already make weight management harder, stress can amplify these difficulties significantly.
Many women notice they gain weight around their midsection during this period, even without eating more. Others find themselves reaching for comfort foods more frequently or feeling unable to control cravings despite their best intentions.
This article examines how stress hormones interact with menopausal changes to promote weight gain, particularly abdominal fat accumulation. You’ll learn practical, evidence-based strategies for managing stress and reducing emotional eating to support your weight management goals during this transition.
What the Stress-Weight Connection Actually Is
The relationship between stress and weight gain centers on cortisol, often called the “stress hormone.” When you experience stress—whether physical, emotional, or psychological—your adrenal glands release cortisol as part of your body’s survival response.
In short bursts, cortisol is protective and necessary. It mobilizes energy, sharpens focus, and helps you respond to threats. The problem emerges with chronic stress, which keeps cortisol elevated for extended periods.
This stress-weight connection isn’t about willpower or discipline. It’s a physiological response driven by hormones that influence appetite, metabolism, and fat storage patterns. Understanding this helps remove self-blame and focus on addressing the underlying mechanisms.
During menopause, this dynamic becomes more pronounced because declining estrogen already affects weight regulation. When chronic stress adds elevated cortisol to the mix, the combined effect creates a particularly challenging environment for weight management.
Why This Matters During Menopause
The menopausal transition often coincides with significant life stressors: aging parents requiring care, children leaving home, career pressures, or relationship changes. These stressors occur precisely when hormonal changes make the body more vulnerable to stress-related weight gain.
The Perfect Storm Effect
Menopause creates what some practitioners describe as a “perfect storm” for stress-related weight gain:
- Declining estrogen alters fat distribution, favoring abdominal storage
- Reduced estrogen may impair the body’s ability to manage cortisol effectively
- Sleep disruption from menopausal symptoms elevates stress hormones
- The stress response itself becomes more pronounced with age
Health Implications Beyond Weight
Stress-related abdominal fat accumulation poses specific health risks. This visceral fat (fat surrounding internal organs) is metabolically active and increases risk for:
- Cardiovascular disease
- Type 2 diabetes
- Inflammatory conditions
- Metabolic syndrome
Managing stress during menopause isn’t just about weight—it’s about protecting long-term health.
Key Mechanisms: How Stress Affects Your Weight
Understanding the specific ways stress influences weight helps you target interventions more effectively.
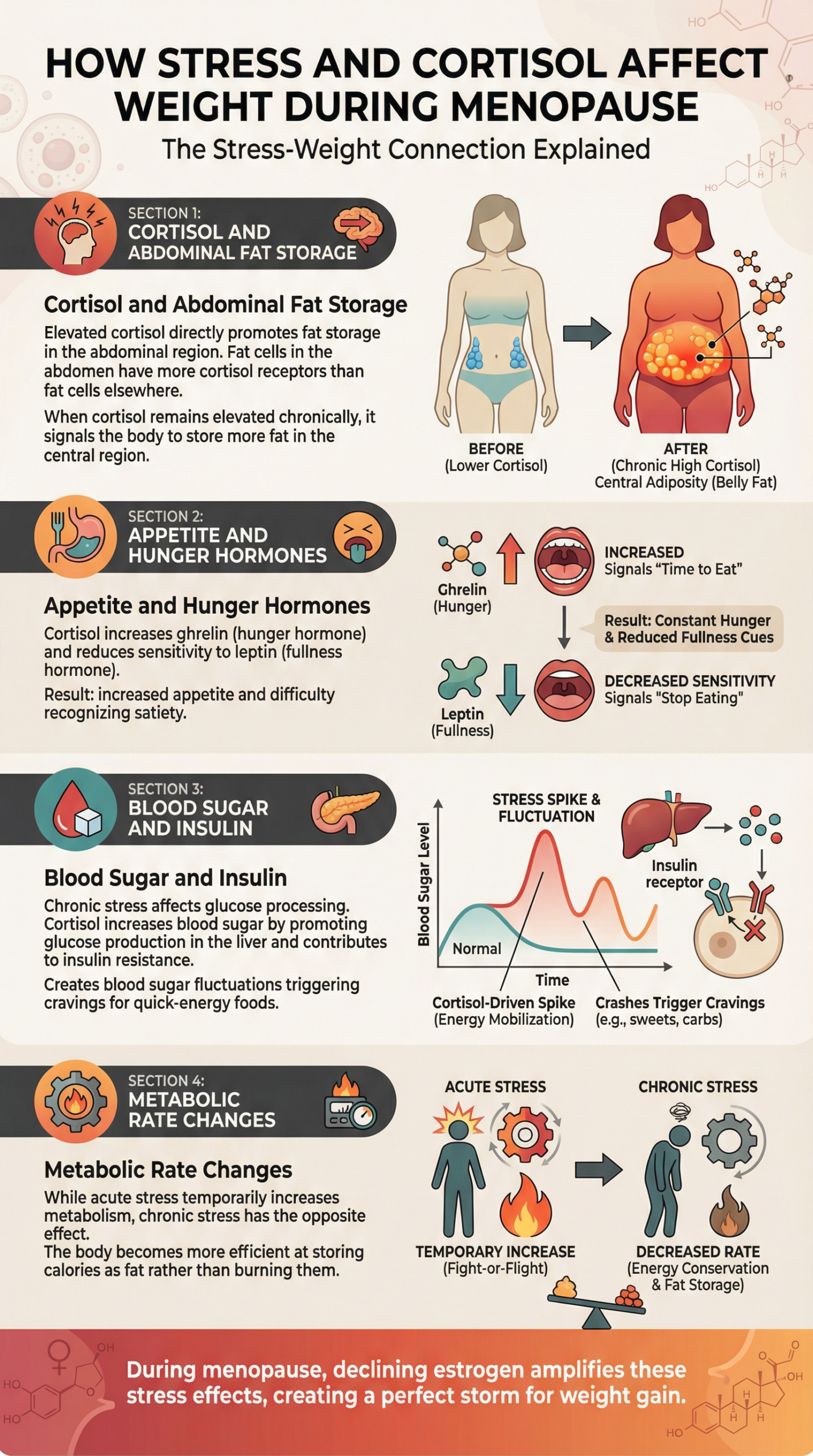
Cortisol and Abdominal Fat Storage
Elevated cortisol directly promotes fat storage in the abdominal region. Fat cells in the abdomen have more cortisol receptors than fat cells elsewhere, making this area particularly responsive to stress hormones.
When cortisol remains elevated chronically, it signals the body to store more fat in this central region. This explains why stressed individuals often gain weight specifically around their midsection, even if their overall weight doesn’t change dramatically.
Appetite and Hunger Hormones
Cortisol influences the hormones that regulate hunger and fullness:
- It can increase levels of ghrelin, the hormone that triggers hunger
- It may reduce sensitivity to leptin, the hormone that signals fullness
- The result: increased appetite and difficulty recognizing satiety
Many women report feeling hungrier during stressful periods and finding it harder to feel satisfied after eating. This isn’t a failure of willpower—it’s a hormonal response to stress.
Blood Sugar and Insulin
Chronic stress affects how your body processes glucose. Cortisol can:
- Increase blood sugar levels by promoting glucose production in the liver
- Contribute to insulin resistance over time
- Create blood sugar fluctuations that trigger cravings for quick-energy foods
This mechanism explains why stressed individuals often crave sugary or high-carbohydrate foods—the body seeks rapid glucose to respond to perceived threats.
Cravings for Specific Foods
Stress doesn’t just increase appetite generally; it shifts food preferences toward specific types. Elevated cortisol increases cravings for:
- High-sugar foods
- High-fat foods
- Foods that combine both (like ice cream, pastries, or fast food)
These “comfort foods” temporarily reduce stress by triggering pleasure centers in the brain. However, this creates a cycle where stress drives eating, followed by temporary relief, followed by guilt and more stress.
Metabolic Rate Changes
Chronic stress can slow metabolic rate over time. While acute stress temporarily increases metabolism, ongoing stress has the opposite effect, making the body more efficient at storing calories as fat rather than burning them.
Step-by-Step: Managing Stress to Support Weight Goals

Addressing stress-related weight gain requires targeting both the stress itself and the eating patterns it triggers.
1. Identify Your Stress Triggers
Begin by recognizing what specifically triggers stress in your life:
- Work deadlines or conflicts
- Family responsibilities or caregiving
- Financial concerns
- Relationship issues
- Health worries
- Social obligations
Keep a brief stress journal for one week, noting when you feel most stressed and what preceded those feelings. This awareness helps you anticipate and prepare for high-stress situations.
2. Implement Daily Stress-Reduction Practices
Regular stress management works better than reactive approaches. Choose practices you can sustain:
Physical Activity: Exercise directly reduces cortisol levels and improves stress resilience. Both aerobic exercise and strength training provide benefits. Aim for at least 30 minutes most days.
Mindfulness and Meditation: Even brief practices (5-10 minutes daily) can lower cortisol and improve stress responses. Options include guided meditation apps, breathing exercises, or body scan techniques.
Adequate Sleep: Poor sleep elevates cortisol and worsens stress responses. Prioritize 7-8 hours nightly with consistent sleep and wake times.
Social Connection: Meaningful social interaction with supportive people reduces stress hormones and provides emotional buffering against stressors.
3. Recognize Emotional Eating Patterns
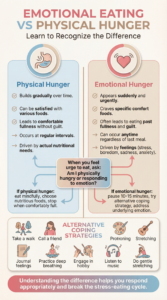
Emotional eating—eating in response to feelings rather than physical hunger—becomes more common under stress. Learning to distinguish between physical hunger and emotional eating is crucial.
Physical hunger:
- Builds gradually
- Can be satisfied with various foods
- Leads to comfortable fullness without guilt
Emotional hunger:
- Appears suddenly
- Craves specific comfort foods
- Often leads to eating past fullness and subsequent guilt
When you notice the urge to eat, pause and ask: “Am I physically hungry, or responding to an emotion?”
4. Develop Alternative Coping Strategies
Create a list of non-food responses to stress and difficult emotions:
- Take a 10-minute walk
- Call a friend
- Practice deep breathing for 5 minutes
- Engage in a hobby or creative activity
- Take a warm bath
- Listen to music
- Write in a journal
Having prepared alternatives makes it easier to choose them when stress strikes.
5. Structure Your Eating Patterns
Regular, balanced meals help stabilize blood sugar and reduce stress-driven cravings:
- Eat at consistent times daily
- Include protein with each meal to promote satiety
- Don’t skip meals, which can trigger increased cortisol
- Plan healthy snacks for predictable stress times
6. Practice Mindful Eating
When you do eat, minimize distractions and focus on the experience:
- Eat slowly, chewing thoroughly
- Notice flavors, textures, and aromas
- Check in with hunger and fullness signals mid-meal
- Stop eating when comfortably satisfied, not stuffed
This practice helps break automatic eating patterns and reconnects you with your body’s natural hunger and fullness cues.
Common Pitfalls and How to Avoid Them
Pitfall: All-or-Nothing Thinking
Believing one stress-eating episode means you’ve “failed” often leads to giving up entirely or continuing to overeat (“I already ruined it, so…”).
Solution: Treat each eating occasion separately. One instance of emotional eating doesn’t define your overall pattern. Return to your plan at the next meal without self-punishment.
Pitfall: Eliminating All Comfort Foods
Completely forbidding foods you find comforting can increase their psychological power and lead to eventual overindulgence.
Solution: Allow moderate portions of preferred foods in a planned, mindful way rather than during high-stress moments when control is harder.
Pitfall: Relying Only on Willpower
Trying to “power through” stress without addressing it directly eventually depletes mental resources, making emotional eating more likely.
Solution: Actively manage stress using multiple strategies rather than depending on willpower alone to resist stress-triggered cravings.
Pitfall: Perfectionist Stress Management
Adding stress about “doing stress management perfectly” defeats the purpose.
Solution: Start with one or two manageable practices. Even imperfect implementation provides benefits. Build from there.
Different Approaches: Finding What Works for You
No single stress-management approach works for everyone. Consider these options and their tradeoffs:
Structured Programs vs. Flexible Approaches
Structured programs (like mindfulness-based stress reduction courses) provide guidance and accountability but require time commitment. Flexible, self-directed approaches offer convenience but need self-discipline.
Consider starting with structured support if you’re new to stress management, then transitioning to flexible maintenance.
Individual vs. Group Support
Working with a therapist, counselor, or health coach provides personalized attention and addresses specific issues. Group programs or classes offer community support and cost-effectiveness.
Some women benefit from combining both: professional help for underlying issues plus group support for ongoing motivation.
Eastern vs. Western Approaches
Practices like yoga, tai chi, and meditation offer holistic approaches rooted in Eastern traditions. Western approaches might include cognitive-behavioral therapy or biofeedback.
Both have evidence supporting effectiveness. Choose based on what resonates with your preferences and beliefs.
Technology-Assisted vs. Traditional Methods
Apps and wearables can track stress, guide meditation, or provide biofeedback. Traditional methods like journaling, talking with friends, or spending time in nature require no technology.
Technology offers convenience and data tracking but may not suit everyone. Many find a hybrid approach most sustainable.
Practical Implementation Checklist
- Complete a one-week stress journal identifying your main triggers
- Choose 2-3 stress-management practices you can commit to daily
- Schedule these practices at specific times (morning, lunch break, evening)
- Create a list of 5-7 non-food stress responses you can use anytime
- Plan regular, balanced meals at consistent times
- Identify one social connection you’ll nurture weekly
- Set a realistic sleep schedule supporting 7-8 hours nightly
- Before eating, practice the “Am I physically hungry?” check
- Keep a brief log of emotional eating episodes to identify patterns
- Celebrate small successes in stress management, not just weight changes
Frequently Asked Questions
Can I reduce cortisol through diet alone?
While certain dietary patterns may support healthy cortisol levels, diet alone typically isn’t sufficient for managing chronic stress. A comprehensive approach including stress-reduction practices, sleep, and physical activity produces better results.
How long does it take to see weight changes after improving stress management?
This varies individually. Some women notice reduced cravings and easier appetite control within a few weeks. Actual weight changes typically become apparent over 2-3 months of consistent stress management combined with appropriate eating patterns.
Will stress always trigger emotional eating once it’s become a habit?
No. While established patterns feel automatic, new responses can be learned. With consistent practice using alternative coping strategies, the association between stress and eating weakens over time.
Should I avoid all stress during menopause?
Completely avoiding stress is neither possible nor necessary. The goal is managing chronic, excessive stress and developing healthy responses. Some stress (eustress) from positive challenges can actually be beneficial.
Can reducing stress help with other menopausal symptoms besides weight?
Yes. Effective stress management often improves sleep quality, reduces hot flash severity, stabilizes mood, and enhances overall quality of life during menopause. Weight management is one of multiple benefits.
Do I need professional help or can I manage this on my own?
Many women successfully implement stress-management strategies independently, especially with clear guidance. However, if stress feels overwhelming, interferes significantly with daily life, or involves symptoms of anxiety or depression, professional support from a therapist or counselor is valuable.
Conclusion
The connection between stress and weight gain during menopause is physiological, not a personal failing. Elevated cortisol affects appetite hormones, food preferences, fat storage patterns, and metabolism in ways that promote weight gain, particularly around the abdomen.
Key takeaways:
- Chronic stress elevates cortisol, which directly promotes abdominal fat storage and increases cravings for high-calorie comfort foods
- The combination of menopausal hormonal changes and chronic stress creates particularly challenging conditions for weight management
- Effective stress management requires addressing the stress itself, not just trying to resist stress-driven eating through willpower alone
- Multiple strategies work together more effectively than any single approach: stress reduction, regular eating patterns, physical activity, adequate sleep, and alternative coping skills
- Learning to distinguish physical hunger from emotional eating helps break automatic stress-eating patterns
Your next step: Choose one stress-management practice from this article that feels doable and commit to it for two weeks. Pair it with identifying one common stress trigger and planning a specific non-food response. Small, consistent changes in stress management create the foundation for sustainable progress in weight management during menopause.