Introduction
Intermittent fasting (IF) has emerged as a popular dietary approach, often praised for its potential weight loss and metabolic benefits. However, a growing body of evidence suggests that its impact extends beyond physical health, influencing mental well-being, focus, clarity, and mood regulation. This article explores the science behind intermittent fasting’s effects on the brain, providing a balanced, evidence-based perspective on its potential benefits and considerations for mental health.
The Science Behind Intermittent Fasting and the Brain
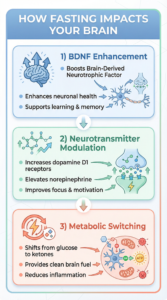
Intermittent fasting is not merely about calorie restriction; it’s a strategic eating pattern that triggers a cascade of metabolic and cellular changes. One of the most significant is metabolic switching, where the body transitions from using glucose as its primary fuel source to burning ketone bodies derived from fat. This switch has profound implications for brain health.
Brain-Derived Neurotrophic Factor (BDNF)
Fasting has been shown to increase the production of Brain-Derived Neurotrophic Factor (BDNF), a protein crucial for neuronal survival, growth, and synaptic plasticity . Often described as “Miracle-Gro for the brain,” BDNF plays a vital role in learning, memory, and higher-order thinking. Enhanced BDNF levels may explain the reports of increased mental clarity and focus during fasting periods.
Neurotransmitter Modulation
Recent research has uncovered a direct link between intermittent fasting and neurotransmitter systems, particularly dopamine. A 2025 study published in Neurobiology of Disease found that IF produces antidepressant-like effects by modulating dopamine D1 receptors in the medial prefrontal cortex . This suggests that fasting can positively influence mood and motivation by enhancing dopamine signaling.
Furthermore, fasting is associated with increased concentrations of norepinephrine and epinephrine, which can enhance alertness and focus .
The Impact on Mental Well-Being
While the initial adaptation period to intermittent fasting can be challenging, many individuals report significant improvements in mental well-being once their bodies adjust. Here’s a breakdown of the potential effects:
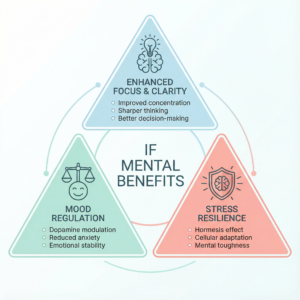
Focus and Clarity
Contrary to the belief that fasting impairs cognitive function, a 2025 meta-analysis by the American Psychological Association concluded that short-term fasting (less than 24 hours) does not impair mental performance in healthy adults . In fact, many people experience heightened focus and clarity, likely due to:
•Increased BDNF: Promotes neuronal health and cognitive function.
•Ketone Utilization: The brain can efficiently use ketones for energy, which may lead to more stable cognitive performance.
•Reduced Inflammation: Fasting can lower systemic inflammation, which is linked to cognitive fog and impairment.
Mood Regulation
The connection between intermittent fasting and mood is complex but promising. The antidepressant-like effects observed in animal studies are attributed to the modulation of dopamine receptors . By enhancing dopamine signaling, IF may help alleviate symptoms of anhedonia (the inability to feel pleasure) and improve overall mood.
However, it’s important to note that some individuals may experience mood swings, irritability, or anxiety during the initial 2-4 week adaptation period. These symptoms typically subside as the body becomes more efficient at using fat for fuel.
Stress Resilience
Intermittent fasting can be viewed as a form of hormesis—a beneficial type of stress that strengthens the body’s ability to cope with more significant stressors. By activating cellular stress-response pathways, IF can enhance neuroendocrine activation and improve the body’s resilience to both physiological and psychological stress .
Practical Tips for Maintaining Mental Well-Being During Fasting
Successfully integrating intermittent fasting into your lifestyle requires a mindful approach that prioritizes mental well-being. Here are some practical tips:
1. Start Slowly and Choose the Right Method
•16/8 Method: This is the most popular and beginner-friendly approach, involving a 16-hour fast and an 8-hour eating window. It’s a great starting point to ease your body into fasting.
•5:2 Method: This method offers more flexibility, with five days of normal eating and two non-consecutive days of restricted calories (500-600).
•Listen to Your Body: Pay attention to how you feel and adjust your fasting schedule as needed. There is no one-size-fits-all approach.
2. Prioritize Nutrient-Dense Foods
During your eating window, focus on consuming high-quality, nutrient-dense foods to support brain health and stabilize mood. Include:
•Healthy Fats: Avocado, nuts, seeds, and olive oil.
•Lean Proteins: Fish, chicken, beans, and lentils.
•Complex Carbohydrates: Whole grains, fruits, and vegetables.
•Hydration: Drink plenty of water, herbal tea, or black coffee throughout the day.
3. Manage Stress Proactively
Since fasting is a form of stress, it’s crucial to manage other stressors in your life. Incorporate stress-reduction techniques such as:
•Mindfulness and Meditation: Even 10-15 minutes a day can make a significant difference.
•Deep Breathing Exercises: Activate the parasympathetic nervous system to promote relaxation.
•Time in Nature: Spending time outdoors has been shown to reduce cortisol levels and improve mood.
4. Optimize Your Sleep
Sleep is critical for mental well-being, especially during fasting. Aim for 7-9 hours of quality sleep per night. Establish a consistent sleep schedule and create a relaxing bedtime routine to signal to your body that it’s time to wind down.
5. Be Patient with the Adaptation Period
It can take 2-4 weeks for your body to adapt to intermittent fasting. During this time, you may experience fatigue, headaches, or moodiness. Be patient with yourself and support your body with adequate hydration, nutrition, and rest.
6. Build a Support System
Having accountability and support can significantly enhance your mental well-being during the fasting journey. Consider joining online communities, finding a fasting buddy, or working with a healthcare professional who understands your goals. Sharing experiences and challenges with others can provide motivation and practical insights.
Understanding the Mental Health Timeline
The mental health benefits of intermittent fasting don’t appear overnight. Understanding the typical timeline can help set realistic expectations:
Weeks 1-2: This is often the most challenging period. Your body is adjusting to new eating patterns, and you may experience hunger, irritability, and difficulty concentrating. These symptoms are temporary and typically resolve as your body adapts.
Weeks 3-4: As metabolic switching occurs, many people report improved energy levels and mental clarity. Mood often stabilizes as the body becomes more efficient at using fat for fuel.
Weeks 5-8: By this point, most people experience the full benefits of IF, including improved focus, enhanced mood, and greater emotional resilience. The adaptation period is complete, and fasting becomes a more natural part of your routine.
Beyond 8 Weeks: Long-term practitioners often report sustained mental health benefits, including improved stress resilience, better emotional regulation, and enhanced cognitive performance.
Recognizing When to Seek Professional Help
While intermittent fasting can support mental well-being, it’s important to recognize when professional guidance is necessary. You should consult with a healthcare professional if you:
•Experience persistent mood swings, anxiety, or depression beyond the initial 4-week adaptation period.
•Have a history of eating disorders or disordered eating patterns.
•Are pregnant or breastfeeding.
•Have diabetes or other blood sugar regulation issues.
•Are taking medications that need to be taken with food.
•Have been diagnosed with a mental health condition such as bipolar disorder, depression, or anxiety disorder.
•Experience severe fatigue, dizziness, or cognitive impairment that doesn’t improve after 4 weeks.
Intermittent fasting can be a powerful tool for mental well-being, but it should complement, not replace, professional mental health treatment when needed.
Conclusion
Intermittent fasting is more than just a weight loss tool; it’s a powerful dietary strategy that can have a profound impact on mental well-being. By promoting metabolic switching, enhancing BDNF production, and modulating neurotransmitter systems, IF offers a promising avenue for improving focus, clarity, and mood regulation.
However, it’s essential to approach intermittent fasting with a mindful, evidence-based perspective. By starting slowly, prioritizing nutrient-dense foods, managing stress, and optimizing sleep, you can harness the mental health benefits of IF while supporting your overall well-being. As with any significant lifestyle change, patience, self-compassion, and professional guidance are the keys to long-term success.





